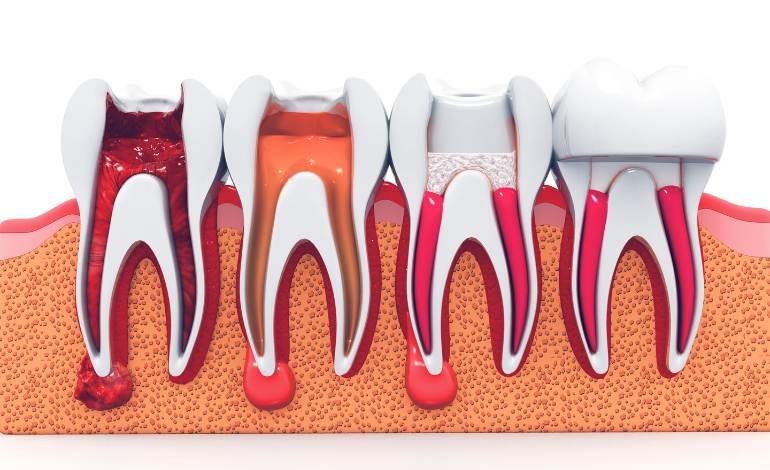
6 Signs of Infection After Root Canal Treatment
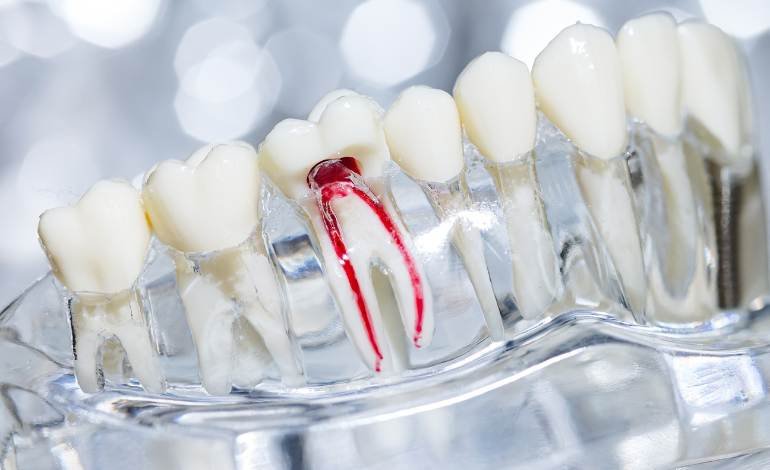
A root canal treatment is done to remove infected or inflamed tissue from inside a tooth, clean the root canals, and seal the tooth so it can be saved. Most root canal-treated teeth heal well, especially when the final filling or crown is completed on time. But in some cases, infection can remain, return, or develop around the root after treatment.
The early signs of infection after root canal treatment can be easy to miss. Some soreness after a root canal is normal, but severe pain, swelling, pus, fever, a bad taste, or a loose tooth are not signs you should ignore. The American Association of Endodontists advises patients to contact their dentist or endodontist if they have severe pain or pressure lasting more than a few days, visible swelling, an uneven bite, loss of a temporary filling or crown, or return of symptoms after root canal treatment.
This guide explains the 6 signs of infection after root canal treatment, why they happen, and when to contact your dentist.
Understanding Root Canal Infections
A root canal infection can happen when bacteria remain inside the tooth, enter through a leaking filling or crown, or spread around the root tip. Sometimes the infection was already severe before treatment, so the surrounding bone and gum need more time to heal.
Why Infection Can Happen After a Root Canal
Root canals are very detailed procedures. Teeth can have narrow canals, curved roots, hidden branches, cracks, or old restorations that make treatment more complex. If bacteria remain in hard-to-reach areas, symptoms may return.
Infection can also happen if the tooth is not sealed properly after treatment. A temporary filling that falls out, a delayed crown, or a cracked tooth can allow bacteria to enter again.
Normal Healing vs Infection
Mild tenderness for a few days after a root canal can be normal. The tissues around the tooth may feel sore, especially when chewing. But normal healing should slowly improve.
A possible root canal infection usually feels different. Pain may get worse instead of better. Swelling may appear. A pimple-like bump may form on the gum. You may notice pus, fever, or a bad taste. Cleveland Clinic lists root canal-related infection signs such as a gum boil that may ooze pus, swollen jaw, darkened tooth color, loose tooth, pain spreading to the jaw or face, pain when chewing, and swollen gums.
Sign 1: Unusual Taste Sensations
An unusual taste after a root canal can be an early warning sign, especially if it is bitter, salty, metallic, foul, or keeps coming back.
Why a Bad Taste Can Happen
A bad taste may happen when fluid, bacteria, or pus drains from an infected area near the tooth root. Sometimes a small gum bump opens and releases drainage. This can create a bitter or unpleasant taste in the mouth.
This does not always come with severe pain. In fact, some people feel less pressure after drainage starts. But that does not mean the infection has healed. It means the infection has found a way to drain.
When Taste Changes Are More Concerning
A temporary strange taste can happen from dental materials, medication, or mouth rinses. But a persistent bad taste with gum swelling, bad breath, pain, or pus needs dental attention.
Cleveland Clinic lists bad breath or a bitter taste as symptoms of an abscessed tooth, along with gum redness, swelling, loose tooth, jaw swelling, swollen lymph nodes, a draining sore, and fever.
What You Should Do
Rinse gently with warm salt water to keep the area clean, but do not try to squeeze the gum or drain it yourself. Contact your dentist and explain the taste, when it started, and whether you notice swelling or discharge.
Sign 2: Persistent or Worsening Pain
Some pain after a root canal can be part of healing. But persistent pain after root canal treatment or pain that gets worse is a warning sign.
What Normal Post-Treatment Soreness Feels Like
Normal soreness is usually mild to moderate. It may happen when biting or touching the tooth. It should improve over a few days.
This soreness often comes from inflammation around the root, especially if the tooth was painful before treatment.
What Infection Pain Feels Like
Pain linked with infection may be throbbing, deep, constant, or spreading. It may travel to the jaw, ear, temple, face, or nearby teeth. It may also become worse when lying down or chewing.
Mayo Clinic explains that a tooth abscess may cause severe, constant, throbbing toothache that can spread to the jawbone, neck, or ear. Other symptoms can include chewing pain, fever, swelling, swollen lymph nodes, and bad odor in the mouth.
Pain When Biting
Pain when biting after a root canal may be caused by infection, inflammation around the root, a cracked tooth, or a high temporary or permanent filling. If the bite feels uneven, the tooth may be taking too much pressure.
The AAE specifically advises contacting the dental provider if the bite feels uneven after root canal treatment.
What You Should Do
Do not keep chewing on the painful tooth. Avoid hard foods and call your dentist. The solution may be a bite adjustment, medication inside the tooth, drainage, retreatment, or further imaging.
Sign 3: Swelling and Visible Gum Changes
Swelling after root canal treatment is one of the clearest signs that you should contact your dentist. Swelling may appear around the gum, cheek, jaw, or face.
Gum Swelling Around the Treated Tooth
The gum near the treated tooth may look red, puffy, shiny, or tender. You may notice a raised bump or swelling near the root area.
A small gum bump can be a sinus tract, which is a drainage path from infection. It may look like a pimple on the gum.
Facial or Jaw Swelling
Facial swelling after a root canal is more serious than mild gum tenderness. It may mean infection is spreading beyond the tooth area.
Mayo Clinic states that fever and swelling in the face may require prompt dental care, and if swelling is linked with trouble breathing or swallowing, emergency care is needed.
Swelling That Comes and Goes
Some patients notice swelling that disappears and returns. This can happen when infection drains temporarily and then builds again. Do not ignore it just because it reduces for a while.
What You Should Do
Call your dentist if you see swelling inside or outside the mouth. If swelling spreads quickly, reaches the eye or neck, or affects swallowing or breathing, seek urgent medical care.
Sign 4: Fever and Systemic Symptoms
A dental infection can sometimes affect more than the tooth. Fever after root canal treatment, chills, fatigue, swollen lymph nodes, or feeling generally unwell may mean the body is fighting infection.
Why Fever Matters
Fever suggests the infection may not be limited to one small area. It may be spreading or triggering a stronger immune response.
This is not something to manage with painkillers alone. You need professional evaluation.
Other Systemic Symptoms
You may feel tired, weak, achy, or unwell. The lymph nodes under your jaw or in your neck may feel swollen or tender. You may also have difficulty opening your mouth or chewing.
NHS guidance on dental abscesses lists symptoms such as swollen face or jaw, swollen glands, high temperature, bad taste, and difficulty opening the mouth or chewing.
When It Becomes Urgent
Fever with facial swelling is a red flag. Fever with trouble breathing, trouble swallowing, confusion, or rapidly spreading swelling should be treated as urgent.
What You Should Do
Contact your dentist immediately. If symptoms are severe or spreading, seek emergency care. Antibiotics may be needed in some cases, but they do not replace dental treatment if the infection source remains.
Sign 5: Drainage and Pus Formation
Pus after root canal treatment is a strong sign of infection. Pus is the body’s response to bacterial infection and often means an abscess is present.
What Drainage May Look Like
You may notice white, yellow, or cloudy fluid near the gum. It may come from a gum bump, small opening, or swollen area. It may also create a bad taste or bad breath.
Sometimes the gum bump drains, shrinks, and then returns. This cycle can continue until the infection source is treated.
Why Pus Should Never Be Ignored
Pus means bacteria and inflammatory cells are collecting in the tissue. Even if the pain decreases after drainage, the infection is still active.
Mayo Clinic explains that abscess treatment may include draining the abscess, performing a root canal to remove infection, prescribing antibiotics when infection has spread, or extracting the tooth if it cannot be saved.
Do Not Drain It Yourself
Do not press, cut, squeeze, or poke the swollen area. This can spread bacteria or injure the gum.
What You Should Do
Book urgent dental care. The dentist may need to take an X-ray, drain the abscess safely, reopen the tooth, prescribe medication if needed, or consider root canal retreatment.
Sign 6: Tooth Discoloration or Increased Mobility
A tooth that becomes darker or feels loose after treatment should be checked. These signs may suggest infection, trauma, bone loss, or structural damage.
Tooth Discoloration After Root Canal
A root canal-treated tooth can sometimes darken over time, especially if there was trauma or old blood products inside the tooth. Not every color change means active infection, but it should still be examined.
Discoloration with pain, swelling, gum changes, or a bad taste is more concerning.
Loose Tooth After Root Canal
A loose adult tooth is never normal. Infection around the root can weaken the surrounding bone. Gum disease, trauma, or a cracked root can also cause mobility.
Cleveland Clinic lists a loose tooth as one possible sign linked with infection weakening nearby bone.
Cracked Root or Failed Restoration
Sometimes the root canal itself is not the only issue. A cracked tooth, leaking crown, broken filling, or delayed final restoration can allow bacteria back in. This can cause reinfection and mobility.
What You Should Do
See your dentist as soon as possible. The dentist may check the crown or filling, test mobility, take X-rays, and decide whether the tooth can be saved.
Conclusions
The 6 signs of infection after root canal treatment include unusual taste, persistent or worsening pain, swelling, fever, pus, and tooth discoloration or looseness. Mild soreness after treatment can be normal, but these warning signs should not be ignored.
A root canal is meant to save the tooth, remove infection, and protect your oral health. If symptoms return or get worse, the tooth may need further care. That care may include bite adjustment, drainage, medication, retreatment, a new crown or filling, or specialist treatment from an endodontist.
The safest step is simple: contact your dentist early. Fast treatment can reduce pain, stop infection from spreading, and improve the chance of saving your natural tooth.
What Happens During a Root Canal
Learn More
FAQS
Is pain normal after root canal treatment?
Mild soreness can be normal for a few days, especially when biting. But severe pain, worsening pain, or pressure lasting more than a few days should be checked by your dentist.
How do I know if my root canal is infected?
Signs of a root canal infection may include bad taste, swelling, pus, fever, gum pimple, worsening pain, pain when biting, tooth discoloration, or a loose tooth.
Can an infection come back after a root canal?
Yes. Infection can return if bacteria remain in hidden canals, the tooth cracks, the filling or crown leaks, or the final restoration is delayed.
Is pus after a root canal an emergency?
Pus is a sign of infection and should be checked urgently. If pus comes with facial swelling, fever, or trouble swallowing, seek urgent care.
Can antibiotics fix a root canal infection?
Antibiotics may help when infection has spread, but they usually do not remove the source inside or around the tooth. Dental treatment may still be needed.
What happens if I ignore infection after a root canal?
Ignoring infection can lead to worsening pain, abscess, bone loss, spreading infection, and possible tooth loss.
Should I see a dentist or an endodontist?
Start with your dentist. They can examine the tooth and refer you to an endodontist if the case is complex or needs root canal retreatment.